Michael knight review models mark manson
Results Among the 3019 participants in this analysis, all were women with a mean (SD) age of 63.1 (6.8) years at enrollment and 68.5 (7.1) years at diagnosis. Comparisons between groups were made using the t test, the χ 2 test, and Fine-Gray multivariable cumulative incidence regression analyses. Secondary outcomes included prognostic and tumor characteristics for each group. Main Outcomes and Measures The primary outcome of this study was breast cancer–specific mortality for each case of breast cancer detected by screening and IBCs detected within 1 year or between 1 and 2.5 years from a mammogram with negative results. Interval breast cancers were subdivided into those occurring within 1 year or between 1 and 2.5 years after the last protocol-mandated mammogram with negative results. Breast cancers detected by screening and IBCs were defined based on mammogram history, date of last mammogram, type of visit, and results of examination.
Statistical analysis was performed from October 25, 2018, to November 24, 2019.

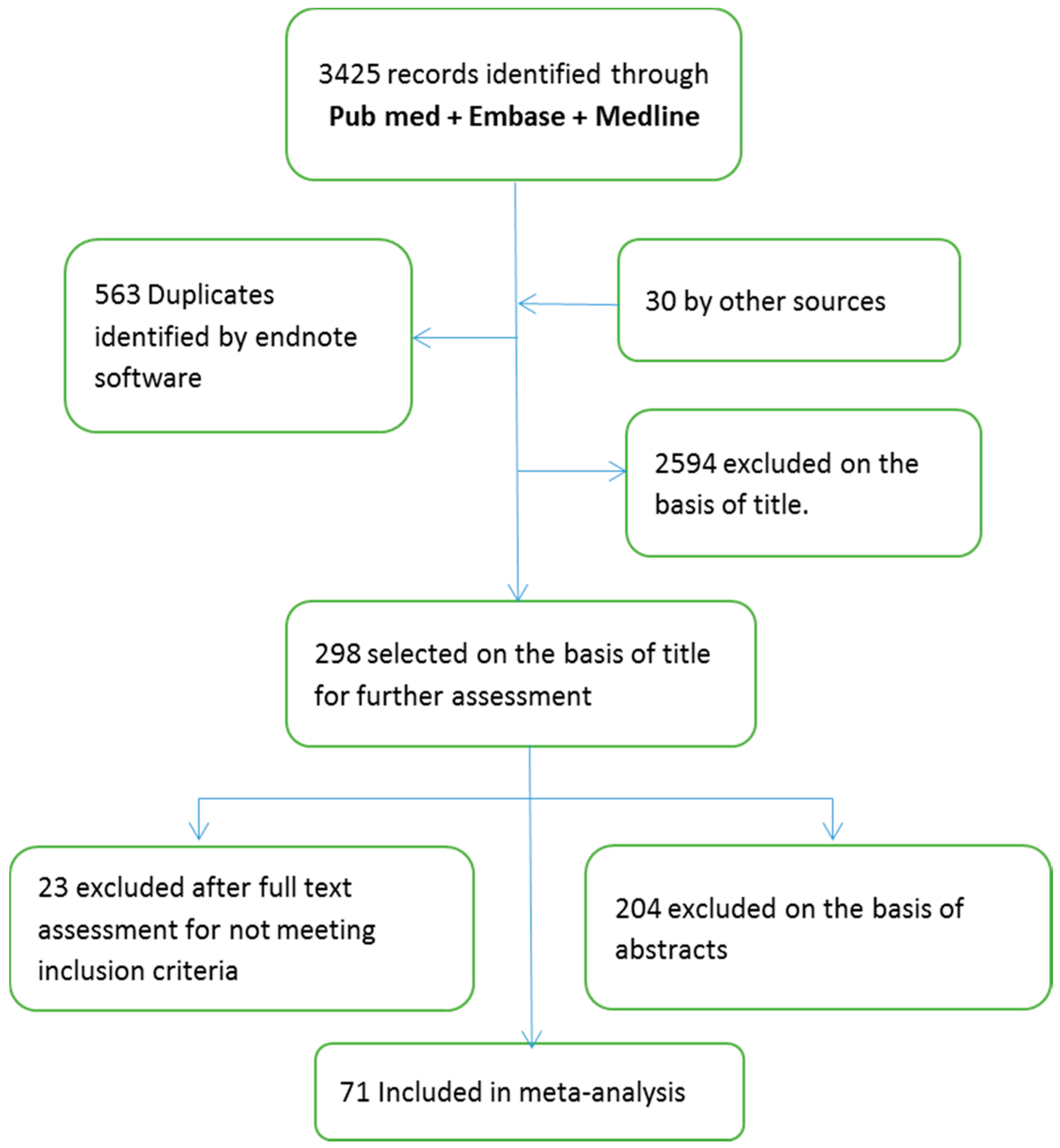
There were 5455 incidents of breast cancer only 3019 women compliant with screening were retained in analyses. The present study sample for these analyses included women aged 50 to 79 years who participated in the Women’s Health Initiative study and includes data collected through March 31, 2018. Objective To compare the prognostic features and mortality rate of women with IBCs diagnosed within 1 year or between 1 and 2.5 years of a mammogram with negative results with the prognostic features and mortality rate of women with breast cancers detected by screening.ĭesign, Setting, and Participants This cohort study used mammography data, tumor characteristics, and patient demographic data from the Women’s Health Initiative study, which recruited participants from 1993 to 1998 and followed up with participants for a median of 19 years. Interval breast cancer has a worse prognosis than cancers detected by screening however, it is unknown whether the length of the interscreening period is associated with prognostic features and mortality. Importance Interval breast cancers (IBCs) are cancers that emerge after a mammogram with negative results but before the patient’s next scheduled screening. Meaning Interval cancers occurring within 1 year from a mammogram with negative results may have a unique biology that accounts for aggressive features.
#Michael knight review models mark manson trial#
Mortality remained statistically significantly higher after adjustment for trial group, molecular subtype, other risk factors, histologic characteristics, and either tumor size or lymph node but not when tumor size and lymph node were included in the model no differences were observed between interval cancers diagnosed between 1 and 2.5 years from a mammogram with negative results and breast cancers detected by screening. Question Is the length of the interscreening period associated with breast cancer prognostic factors and mortality in interval breast cancers compared with cancers detected by screening?įindings In this study using data from the Women’s Health Initiative, a national study among postmenopausal women, interval breast cancers diagnosed within 1 year from a mammogram with negative results were associated with worse breast cancer–specific mortality compared with breast cancers detected by screening.


Multivariate Fine-Gray Competing Risk Models for Breast Cancer–Specific Mortality: Comparison of Interval Breast Cancers and Breast Cancers Detected by Screening After Controlling for Baseline Health and Tumor Characteristics Among Participants in the Control ArmsĮFigure. Multivariate Fine-Gray Competing Risk Models for Breast Cancer–Specific Mortality: Comparison of Interval Breast Cancers and Breast Cancers Detected by Screening After Controlling for Baseline Health and Tumor Characteristics: Replacing the Survival Time From “Diagnosis Date to Death/End-of-Follow-up Date” With “Date of Last Mammogram to Death/End-of-Follow-up Date”ĮTable 5. Multivariate Fine-Gray Competing Risk Models for Breast Cancer–Specific Mortality: Comparison of Interval Breast Cancers and Breast Cancers Detected by Screening After Controlling for Baseline Health and Tumor Characteristics Among Participants Not in HT TrialĮTable 4. Comparison of Tumor Characteristics Between Women With a Diagnosis of Breast Cancer Detected by Screening vs Women With a Diagnosis of Interval Breast Cancer Among Participants Not in HT TrialĮTable 3. Unadjusted Fine-Gray Competing Risk Models for Breast Cancer–Specific MortalityĮTable 2.
